Central Serous Chorioretinopathy
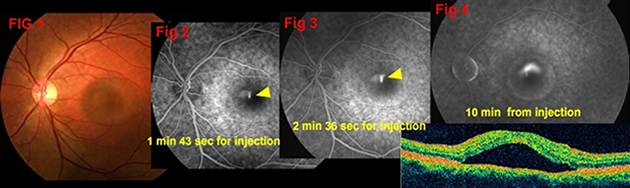
CSR, also known as central serous chorioretinopathy (CSC), is a visual impairment, often temporary, usually in one eye, mostly affecting males in the age group 20 to 50 but which may also affect women. The disorder is characterized by leakage of fluid in the central macula usually with a “blister” appearance (Fig 1), which results in blurred or distorted vision (metamorphopsia). A blind or gray spot in the central vision is common, along with flashes of light (photopsia).
Diagnosis
The diagnosis of CSR usually starts with a dilated examination of the retina, followed with confirmation by fluorescein angiography. The angiography test will usually show one or more fluorescent spots with fluid leakage. In 10%-15% of the cases these will appear in a “classic” smoke stack shape (Figs 2 & 3). An Amsler grid could be useful in documenting the precise area of the visual field involved.
Causes
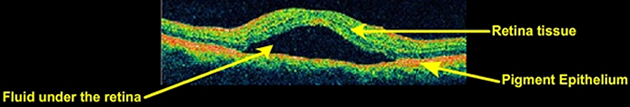
CSR is a fluid detachment of macula layers from their supporting tissue. This allows choroidal fluid to leak into the subretinal space. The buildup of fluid seems to occur because of small breaks in the retinal pigment epithelium. CSR is sometimes called idiopathic CSR which means that its cause is unknown. Nevertheless, stress appears to play an important role. An oft-cited but potentially inaccurate conclusion is that persons in stressful occupations, such as airplane pilots, have a higher incidence of CSR. The “type A personality” has also been linked to this condition. However, the statistics may be skewed by the fact that CSR often goes undiagnosed or misdiagnosed; airline pilots and so-called “type A” people are demonstrably exacting, demanding people with (certainly in the case of pilots) better-than-average vision. They are more likely than the general population to notice the sometimes-subtle degradation of vision caused by CSR and insist on a believable diagnosis of it. People who need glasses may assume that the blurriness caused by CSR is simply a change in their prescription, and fail to have the condition assessed by a retinal specialist. These statistic-skewing factors undermine the conclusion that CSR is a condition specific to “type A” people. CSR has also been associated with cortisol and corticosteroids, and persons with higher levels of cortisol than normal also have a higher propensity to suffer from CSR. Cortisol is a hormone secreted by the adrenal cortex which allows the body to deal with stress, which may explain the CSR-stress association. There is extensive evidence to the effect that corticosteroids (“cortisone”) — commonly used to treat inflammations, allergies, skin conditions and even certain eye conditions — can trigger CSR, aggravate it and cause relapses. The incidence of CSR in persons with Cushing’s syndrome is 5%. Cushing’s syndrome is characterized by very high cortisol levels. Recently found evidence has also implicated Helicobacter pylori (see gastritis) as playing a role. It would appear that the presence of the bacteria is well correlated with visual acuity and other retinal findings following an attack. Recent evidence also shows that sufferers of MPGN Type II kidney disease can develop retinal abnormalities including CSR caused by deposits of the same material that originally damaged the glomerular basement membrane in the kidneys.
Prognosis
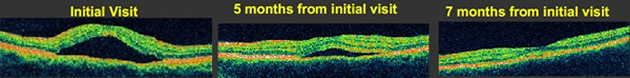
The prognosis for CSR is generally excellent. Over 90% of patients regain 20/30 vision or better within 6 months. Some visual abnormalities can remain even if visual acuity is measured at 20/20. Lasting problems can include decreased night vision, color discrimination problems, and some distortion. Long term complications can include subretinal neovascularization and pigment epitheliopathy.
The OCT images above show the increased fluid under the retina that prompted the initial visit. 5 months later the fluid has significantly decreased and is completly gone after 7 months.
Treatment
There is no known effective treatment for the disease. Laser photocoagulation, which effectively burns the leaking area shut, is sometimes suggested. In many cases the leak is very near the central macula, where photocoagulation would leave a blind spot. Additionally, a better long term outcome has not been demonstrated with photocoagulation. More often than not the condition goes untreated because the break in the retinal pigment epithelium will seal on it’s own and the fluid will subside over time.
Any ongoing corticosteroid treatments should be stopped. Additionally, a new anti-microbial treatment will likely be recommended soon in light of recent findings regarding Helicobacter pylori.CSR sufferers usually find their own ways to manage the condition, which may include stress reduction and changes in nutrition.
